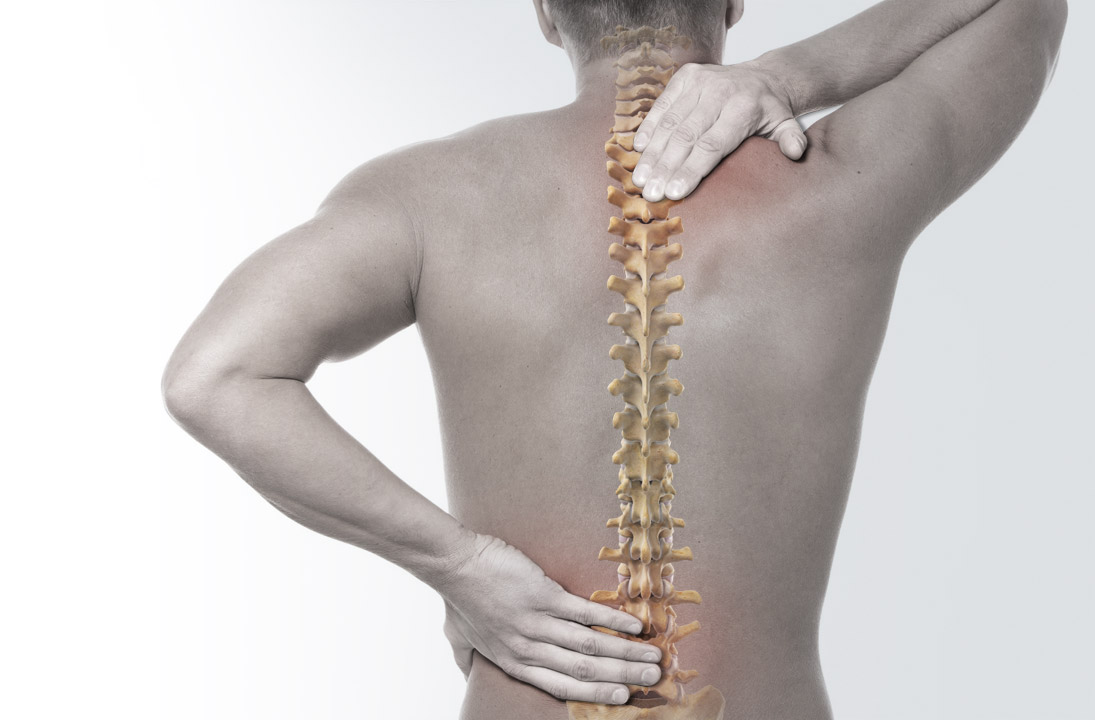
Surgical management of back and leg pain is evolving and changing due to a better understanding of the patho-anatomy well correlated with its pathophysiology. Pain is better understood with in vivo visualization and probing of the pain generators using an endoscopic access rather than just relying on symptoms diagram and image correlation. This has resulted in a shared decision making involving patient and surgeon, focused on a broader spectrum of surgical as well as non-surgical treatments, and not just masking the pain generator. It has moved away from decisions based on diagnostic images alone, that, while noting the image alterations, cannot explain the pain experienced by each individual as images do not always show variations in nerve supply and patho-anatomy. The ability to isolate and visualize “pain” generators in the foramen and treating persistent pain by visualizing inflammation and compression of nerves, serves as the basis for transforaminal endoscopic (TFE) surgery. This has also resulted in better pre surgical planning with more specific and defined goals in mind. The “Inside out” philosophy of TFE surgery is safe and precise. It provides basic access to the disc and foramen to cover a large spectrum of painful pathologies.