- Bryan Cervical Disc
- M6-C *
- Mobi-C *
- PCM Cervical Disc System
- ProDisc-C *
- Secure-C
- Simplify Disc

Cervical artificial disc replacement has exceptionally high success rates that often exceed those of traditional fusion surgery. Success is measured by three factors:
Pain relief
Maintenance of natural motion
Avoiding the need for additional surgery
In 10-year follow-up studies, 98.7% of disc replacement patients reported being very satisfied, compared with 88.9% of fusion patients. For two-level procedures, artificial disc replacement shows significantly lower readmission rates and superior clinical outcomes compared to fusion surgery.
Disc replacement surgery in the neck often surpasses fusion outcomes, especially for patients needing surgery at multiple levels. The key to achieving these excellent results is proper patient selection, as not everyone is a candidate for this motion-preserving surgery.
The ideal candidate for cervical disc replacement has good bone quality but experiences nerve compression symptoms like arm pain, numbness or weakness caused by a damaged disc. You’ll also need healthy facet joints — the small joints at the back of your vertebrae.
Certain conditions make disc replacement unsuitable. If you have significant osteoporosis, the device may not anchor properly in weakened bone. Severe spinal instability, advanced arthritis of the facet joints, or extensive bone spurs may disqualify you as well. In these cases, fusion surgery might be the better choice.
Your surgeon will evaluate your MRI, CT scans, and overall health to determine if you’re a good candidate.
The biggest long-term advantage of artificial disc replacement surgery is the prevention of adjacent segment disease (ASD). This is where the levels above and below a fusion wear out faster due to increased stress. By preserving natural motion, artificial discs protect neighboring disc levels.
Only 2.6% of disc replacement patients develop adjacent segment disease at 5+ years, compared to 16.7% of fusion patients. This dramatic difference means fewer patients need additional surgeries down the road.
Other benefits include faster recovery times and maintained neck mobility. Unlike fusion, where you’re restricted until the bones grow together, disc replacement allows you to gradually return to full activity as your tissues heal.
“In our clinical experience, ideal candidate patients undergoing cervical ADR have a faster return to activity, greater satisfaction, and lower rates of need for additional surgery.”
– Board-Certified Orthopedic Spine Surgeon Dr. Nima Salari
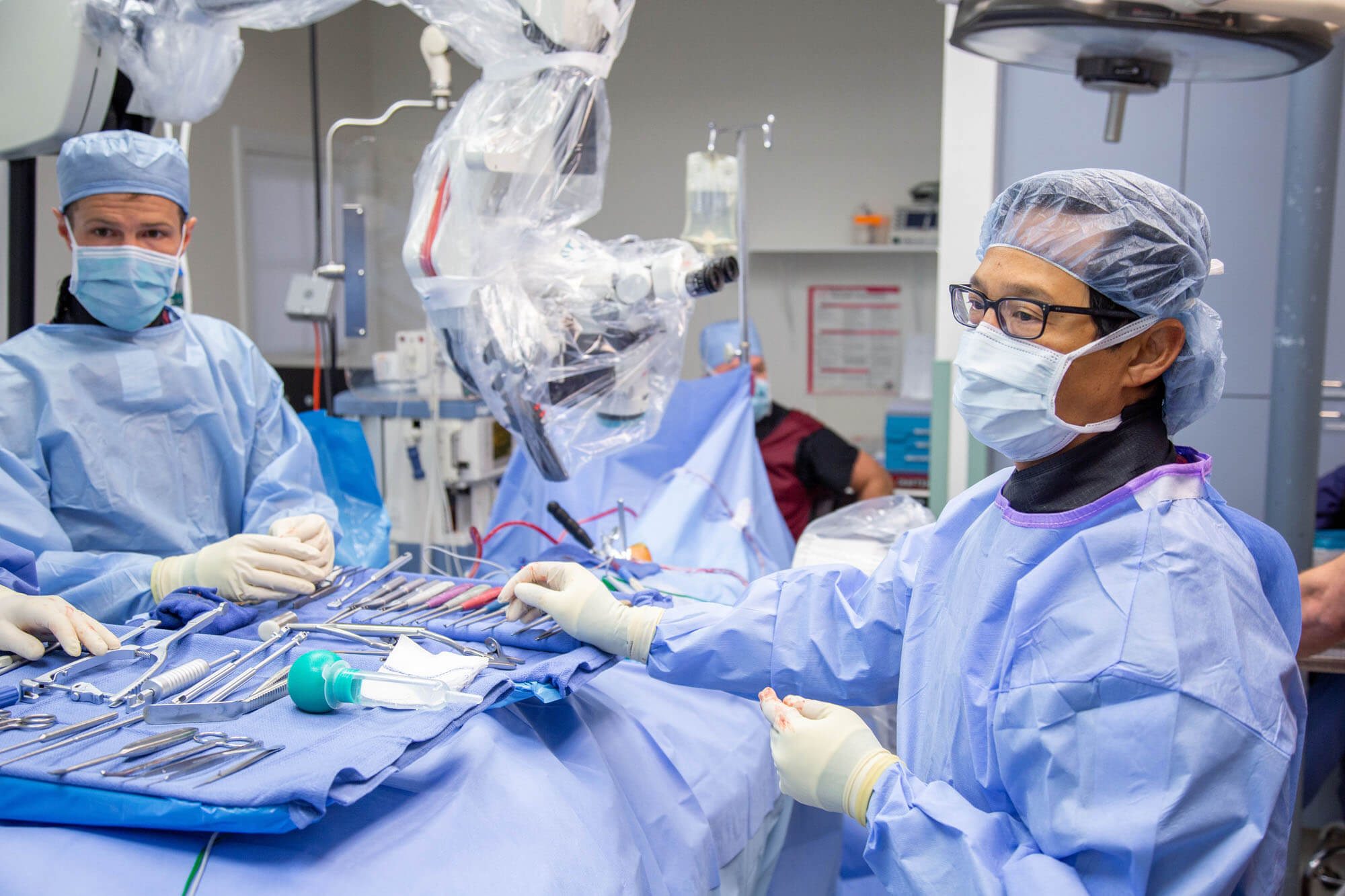
Artificial disc replacement (ADR) is a motion preservation spine surgery that removes a painful damaged spinal disc and replaces it with an artificial disc. This surgery is performed in the low back or the neck.
Cervical artificial disc replacement surgery is performed by a spine surgeon with the
patient under anesthesia. While the patient is asleep lying on their back, the spine surgeon will make a 1- to-2-inch incision on the front of the patient’s neck. The surgeon then removes the affected cervical disc and replaces it with an artificial disc. The surgery lasts about 1-2 hours as an outpatient minimally invasive procedure with patients going home a few hours after surgery.
While the patient is asleep lying on their back, a vascular surgeon assisting the spine surgeon will make a 2-inch incision in the abdomen. The muscle is gently retracted as are the deeper structures including the peritoneal sac and the major blood vessels are moved to the side to create access to the affected lumbar disc. The spine surgeon then removes the damaged degenerative disc and replaces it with an artificial disc. The patient is moved to recovery. The surgery lasts about 2 hours as an outpatient minimally invasive surgery. Most patients go home after a short recovery in the hospital.
Cervical artificial disc replacement surgery will restore your mobility to what it was before surgery. Removing and replacing the painful degenerative disc will relieve the spinal nerves’ pressure, eliminate pain, numbness, and tingling, and significantly improve your quality of life.
After surgery, you should have some pain and discomfort as with any surgery. Patients are discharged from the hospital in a few hours. Your surgeon will provide you with medication to control pain and specific guidelines for return to work and activities when leaving the hospital. Unlike spine fusion surgery, a cervical brace is not usually recommended. Most patients return to work and normal activities between two and six weeks.
Recovery from artificial disc replacement is typically faster than fusion because there’s no need to wait for bones to heal together:
Immediate: Most patients go home the same day or after one night in the hospital. You’ll be able to walk short distances within hours and move your arms and legs to avoid blood clots.
Short-term: Driving is usually allowed once you’re off pain medication and comfortable turning your head, typically within one to two weeks. You will be encouraged to move your neck while your surgeon monitors your progress.
Advanced recovery: Disc replacement patients notice a significant improvement in their quality of life after three to six months. Your surgeon will advise you about a return to exercise like jogging, cycling, and swimming.
As with any surgery, cervical spine surgery has potential risks and complications. There is always the risk for anesthesia complications, allergic reactions, and blood clotting with any spine surgery due to undiagnosed medical conditions such as those related to heart disease.
Potential risks and complications related to any cervical artificial disc replacement surgery may include:
|
|
The latest innovations in artificial disc devices mimic the anatomic structure of a natural disc. Laboratory testing simulates millions of motion cycles — the equivalent of many years of normal use — and shows excellent durability. Clinical data now extends over 10 years, with extremely low rates of device failure or need for removal.
Many of the major insurance carriers cover artificial disc replacement (ADR) based on risks, benefits, and cost of the procedure. However, if your insurance covers ADR, your specific health plan may have restrictions on which patients are approved.
Many insurers still consider cervical disc replacement surgery for degenerative disc disease investigational and experimental and therefore do not cover it. At DISC, our expert spine surgeons are significant advocates of cervical ADR. They often recommend this surgery for suitable candidates.
The limits vary from plan to plan but usually include the following to receive approval:
If you are a candidate, our insurance experts will assist you in getting the surgery approved.
Some health insurance carriers will deny a doctor’s recommendation for a lumbar or cervical artificial disc replacement. Each plan has restrictions on which patients are candidates for approval. When a patient has exhausted all internal and external appeals, they are left with two alternatives. Live with chronic back or neck pain or pay out-of-pocket for spine surgery. If you consider the out-of-pocket expenses, it is essential to understand all of the costs associated with the surgery before moving forward with your surgeon.
The total cost of disc replacement surgery can include the spine surgeon, the anesthesiologist, the vascular surgeon (lumbar surgery), the implant, and the facility’s fees. These fees can be bundled into one or two bills. Make sure to clarify the cost and billing with the surgeon’s office. The total cost of an artificial disc replacement surgery can range from $25,000 to $70,000, with cervical surgery on the lower end and lumbar on the upper end of the price range.
Other costs associated with artificial disc replacement will be pre-operative clearance, including evaluation, bloodwork, X-ray, MRI, and ECG studies. Post-operative, you may need physical therapy or rehabilitation. If paying out-of-pocket, this cost can be charged against your deductible.

Over the past 30 years, there have been a variety of artificial disc replacement devices investigated as an alternative to spinal fusion. This surgical solution is also called spinal arthroplasty or total disc replacement.
The goal of the device is to maintain motion at the surgical level once the damaged disc has been removed and maintain normal biomechanics of the adjacent vertebrae levels above and below the new ADR.
The short answer is yes.
“An artificial disc replacement device may be replaced depending on the presenting symptoms and cause for consideration of the replacement. First, if the device has failed, but the segment is not too arthritic, you could consider a different device. Second, the failed device can be converted to a spinal fusion.” – Dr. Nima Salari
“Yes. Artificial discs can be implanted at multiple levels in the neck. The FDA has approved select disc replacements for two consecutive levels from C3-C7 in the cervical spine.
You may consider additional levels, but there are limited studies, and off-label use of the product is up to the discretion of the spine surgeon in charge of your care.” – Dr. Nima Salari
“Each of the approved artificial disc replacement devices is unique and has many different features. No one device is always the best fit for all patients. We encourage all patients to learn about each device, its makeup, and mechanisms which vary slightly.
Our goal here is not to promote one device over the other. The most common materials used are metal endplates with a polymer like a knee and hip replacement in the middle.” – Dr. Nima Salari

DISC provides comprehensive treatment options spanning non-operative care, ultra-minimal access procedures, mobility-maintaining techniques and minimally invasive approaches for individuals experiencing debilitating spinal and cervical pain conditions.
Our spine health blog features up-to-date spine education and expert spine tips from our spine specialists here at DISC.
1635 East Myrtle Avenue Suite 100, Phoenix, AZ 85020, USA
18700 North 64th Drive Suite 105, Glendale, AZ 85308, USA
8630 East Vía de Ventura Suite 210, Scottsdale, AZ 85258, USA
3487 South Mercy Road, Gilbert, AZ 85297, USA
1635 East Myrtle Avenue Suite 400, Phoenix, AZ 85020, USA