Desert Institute for Spine Care (DISC) is among the pioneers of endoscopic spine surgery, providing our patients with the most advanced technology for better outcomes. We are here to serve our community and beyond with expert spine care for various conditions.
Endoscopic spine surgery (ESS) is a minimally invasive technique to treat spine problems through a tiny, 1/4-inch incision. This procedure uses a small camera and instruments passed through a tube to the target area, guided by X-ray and real-time video. The endoscopic orthopedic procedure allows spine surgeons to operate safely, with greater accuracy, and offer patients better outcomes.
An HD endoscope with an attached HD camera is inserted into the cannula or often called a tubular retractor. The surgeon can now visualize on an HD monitor the spinal canal, vertebral disc and exiting nerves. Endoscopic spine surgery can effectively treat herniated disc, bulging disc, foraminal and stenosis.
Endoscopic surgery is an outpatient procedure, and patients can typically leave within 2 hours after surgery. As a result, patients can benefit from:
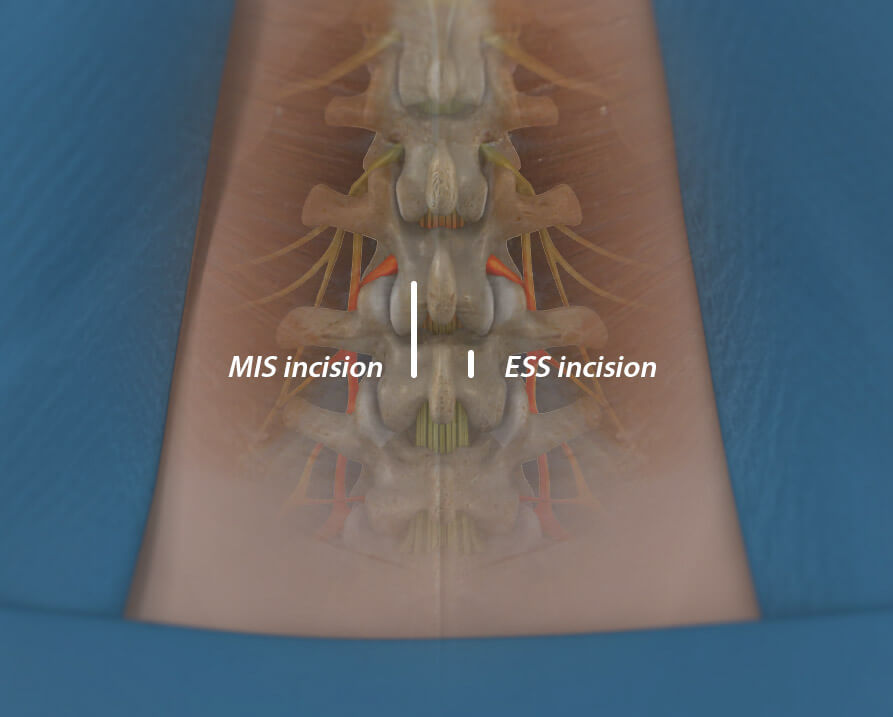
Minimally invasive surgeries (MIS) encompass a wide range of techniques, with endoscopic being the least invasive. In standard MIS techniques, the incision is 1 inch or more, while ESS uses a 1/4-inch incision.
Additionally, endoscopic spine surgery significantly reduces trauma to the patient’s muscles and soft tissue, leading to faster recovery. The endoscopic procedure utilizes a surgical approach that avoids the major stabilizing muscles of the lower back.
Sometimes called ultra-minimally invasive, endoscopic spine surgery can be performed faster, allowing the surgeon better access to the spinal nerves and disc and superior visualization.
Image for illustrative purposes only. Your physician will determine the actual incision placement.
Endoscopic spine surgery aims to decompress or relieve pressure and irritation on the spinal cord and exiting nerve roots, improving pain. Through each of the following options, your endoscopic surgeon will be cautious to preserve spinal anatomy and the function of surrounding muscles:
This is the most common least invasive procedure used to relieve the pressure of a herniated disc on a spinal nerve causing pain. It is also called Selective Endoscopic Discectomy, utilizing the world’s first working channel endoscope to perform direct visualized endoscopic spine surgery.
Endoscopic Facet Medial Branch Nerve Transection is an ultra-minimally invasive endoscopic procedure treating chronic low back pain caused by facet joints in your back. This procedure has been shown to provide up to five years of long-term relief. If you had short-term relief from a pain management radiofrequency ablation procedure, you might be a candidate.
Endoscopic Interlaminar Discectomy is an ultra–minimally invasive procedure that removes herniated disc material through the natural interlaminar window, most often at L5–S1. Using a tiny ¼-inch incision and an HD endoscopic camera, surgeons precisely access and remove the disc fragment with minimal muscle disruption. This technique results in less pain, faster recovery, and a quicker return to normal activity compared to traditional surgery.
This is an ultra-minimally invasive endoscopic laser spine surgery that targets foraminal stenosis, also called lateral recess stenosis. Lateral recess stenosis can be the cause of failed back surgery in up to thirty percent of patients. The endoscopic technique utilizes motorized burrs and a side-firing laser to enlarge the narrow boney foramen, thus relieving the exiting spinal nerve’s pressure. Endoscopic Foraminoplasty may help select patients avoid a minimally invasive spinal fusion.
Endoscopic spine surgery is one of the least invasive surgical options for patients suffering from back and leg pain. Endoscopic spine surgery treats multiple painful spinal conditions, such as:
The ideal candidate for endoscopic spine surgery can vary depending on the specific condition being treated and the surgeon’s assessment. However, in general, the following characteristics may make a patient a good candidate for endoscopic spine surgery:
Our candidate selection process begins with our proprietary Personalized Pain Mapping. Personalized pain mapping of the spine, also known as diagnostic spinal mapping, is a procedure performed to identify and locate the source of a patient’s chronic or persistent spinal pain. It is a diagnostic tool used by spine specialists to gain a better understanding of the specific areas causing pain in an individual patient.
We listen carefully to your pain journey and your desired outcomes. Then we use diagnostic and therapeutic injections to pinpoint the pain generator. We personalize a treatment plan that will effectively address your pain and desired outcomes. Many of our patients get better without any surgical intervention. However, those patients we select for endoscopic spine surgery have great results and a high level of satisfaction.
Personalizing pain mapping of the spine allows for a more accurate diagnosis and helps our expert spine specialists tailor the least invasive and most effective treatment options for patients.
If you think you could benefit from endoscopic spine surgery, our spine specialists can provide you with an accurate spine diagnosis and discuss innovative treatment plans. Schedule your appointment to get started today.
Endoscopic spine surgery is a modern, ultra-minimally invasive technique that allows surgeons to treat common spine conditions through a very small incision — often just a quarter of an inch. Using a tiny camera attached to an endoscope and specialized tools, we can access the problem area with minimal disruption to your muscles and tissues. This means less pain, quicker recovery, and fewer complications compared to traditional surgery.
If you’ve been diagnosed with a herniated disc, spinal stenosis, degenerative disc disease, or even sciatica, there’s a good chance endoscopic spine surgery could help. It’s also an option for people experiencing pain after previous back surgery due to lateral recess stenosis, nerve compression caused by narrowing spaces over the exiting nerve. Many Canadian patients find this option particularly helpful when such techniques are not readily available in their province or region.
Traditional spine surgery often requires a large incision, muscle cutting, and a longer hospital stay. Endoscopic spine surgery, on the other hand, is designed to minimize trauma. The incisions are tiny, there’s much less bleeding, and in most cases, you’ll go home the same day. Recovery is typically faster, and patients often report far less discomfort.
Absolutely! When performed by an experienced and specially trained spine surgeon, endoscopic procedures have an excellent safety record. Like any surgery, there are risks, but serious complications are rare. For out-of-town or out-of-country patients, we also provide post-op care guidance and virtual follow-ups to ensure you feel supported every step of the way.
Most people are surprised at how quickly they feel better. Many return to light activity and administrative work within a week and are back to their regular routines in about a month. Most patients return to physical labor and activities within 4 weeks. Canadian and international patients often appreciate the ability to travel home within a day or two after surgery, with minimal disruption to their life.
All surgeries carry some risks, and endoscopic spine surgery is no exception. Potential issues can include infection, nerve irritation, or a recurrence of symptoms. That said, major complications are uncommon, and we take every precaution to ensure your safety and comfort.
The best candidates are people who have clear evidence of disc or nerve compression—typically confirmed on an MRI—and who haven’t gotten relief from non-surgical treatments like physical therapy, injections, or medications. We offer virtual second opinions for U.S., Canadian, and international patients to review your imaging and determine if you’re a good candidate.
Costs can vary based on a number of factors, including where the surgery is performed, your insurance coverage. On average, the cost ranges from $10,000 to $15,000. We offer transparent pricing and can assist Canadians and international patients with self-pay if their provincial health plan doesn’t cover treatment outside of Canada.
Many U.S. insurance plans—including Medicare—cover endoscopic spine surgery when it’s medically necessary. For Canadian patients, provincial health coverage typically does not pay for care received outside the country. However, we provide documentation and receipts that can help you apply for reimbursement or claim medical expenses.
Start by looking for a board-certified spine surgeon with extensive experience in endoscopic and minimally invasive techniques. Read patient reviews, ask about outcomes, and consider getting a second opinion. Our founder Anthony Yeung, MD (Retired) developed and designed the first endoscopic techniques and surgical instrumentation in the US. He also is responsible for training many of the US and world’s finest spine surgeons. Each of our surgeons at Desert Institute for Spine Care offer endoscopic spine surgery and many are still teaching other surgeons throughout the United States on the weekends. We proudly serve patients across North America and offer virtual consultations for those seeking expert insight before making a decision.
Success rates for endoscopic spine surgery are very promising—especially for patients with conditions like herniated discs and sciatica. In fact, 85% to 95% of individuals report significant pain relief and improved function following their procedure. But it’s important to understand that outcomes can vary depending on a few key factors.
The type of procedure being performed matters. For example, surgeries focused on decompression—such as laminectomies or foraminotomies—may yield different results than fusion surgeries, especially depending on the approach used.
Your personal health profile also plays a role. Younger patients or those in overall good health may recover more quickly, while those with more complex spinal conditions might experience a slower or more variable response. The nature of your diagnosis—like whether it’s a disc herniation, spinal stenosis, or another issue—also impacts success.
Another critical element is the surgeon’s expertise. Choosing a highly experienced, fellowship-trained spine surgeon significantly improves the likelihood of smooth surgery and optimal outcome. Finally, post-operative care can not be overlooked. Patients who carefully follow their recovery plan, including any physical therapy or movement guidelines, tend to heal more efficiently and sustain better long-term results.
In short, while the overall success rate is very high, individual results are shaped by the procedure type, your health, your surgeon, and how closely you follow post-surgical guidance.
Both procedures remove damaged disc material that’s pressing on nerves, but they use different tools and techniques. Endoscopic discectomy is performed through a smaller incision using a camera, while microdiscectomy uses a slightly larger incision and a microscope. Endoscopic methods generally involve less tissue disruption and a quicker recovery. Microscopic typically involves bone resection called a laminectomy in order to access the spine pain generator.
Yes! We use endoscopic tools to relieve pressure on the spinal cord or nerves in cases of lumbar or cervical stenosis. Our surgeons can utilize microscopic instruments and motorized burrs to decompress the boney overgrowth that causes spinal stenosis. It’s a great option for select patients who want to avoid a larger surgery, especially those facing long waitlists in the public health system like Canada.
In most cases, no. Endoscopic spine surgery is typically performed as an outpatient procedure, so you’ll be able to return to your hotel or travel home the same day—often just a few hours after your surgery.
It depends on the kind of work you do. Desk jobs usually require a few days to a week off, while more physical jobs may require up to four weeks of recovery. Your surgeon will help you plan based on your specific situation.
If you’re tired of living with back or neck pain and want to explore whether endoscopic spine surgery is right for you, we’re here to help. Whether you’re in the U.S., Canada, or abroad, our team offers both in-person and virtual consultations—so expert guidance is always within reach.
Our spine health blog features up-to-date spine education and expert spine tips from our spine specialists here at DISC.
1635 East Myrtle Avenue Suite 100, Phoenix, AZ 85020, USA
18700 North 64th Drive Suite 105, Glendale, AZ 85308, USA
8630 East Vía de Ventura Suite 210, Scottsdale, AZ 85258, USA
3487 South Mercy Road, Gilbert, AZ 85297, USA
1635 East Myrtle Avenue Suite 400, Phoenix, AZ 85020, USA