This is the narrowing of the spinal canal, restricting mobility and spinal nerves.
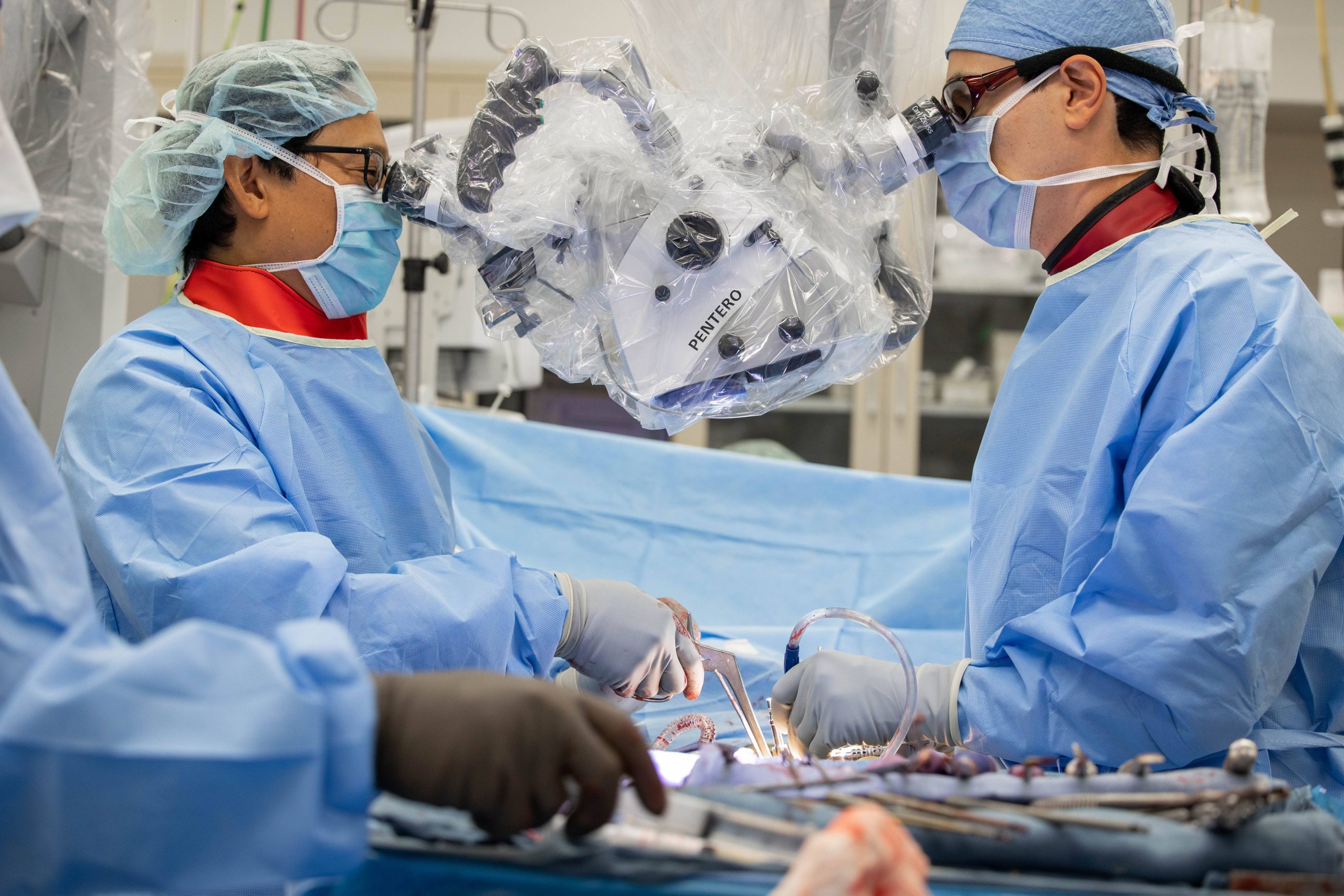
MISS can treat a wide variety of spinal conditions, including:
This is the narrowing of the spinal canal, restricting mobility and spinal nerves.
When the rubbery cushion between your vertebrae becomes irritated and begins to bulge or shift, it puts significant pressure on the spinal canal nerves.
Joint problems in the vertebrae can cause slippage when a vertebra slides forward over the one below.
Spurs are bony projections that grow on the spinal vertebrae and aren’t particularly painful until they affect surrounding tissue and nerves.
Any abnormal spine curvature, usually with one curve like the letter C or two curves like the letter S.
This age-related disease can cause intervertebral disc changes, such as a loss of cushioning, fragmentation and herniation.
Infections in another part of the body can travel to the spinal tissues via the bloodstream.
Several factors can influence sciatica, resulting in a pinched or compressed nerve in the spinal canal’s lower lumbar region.
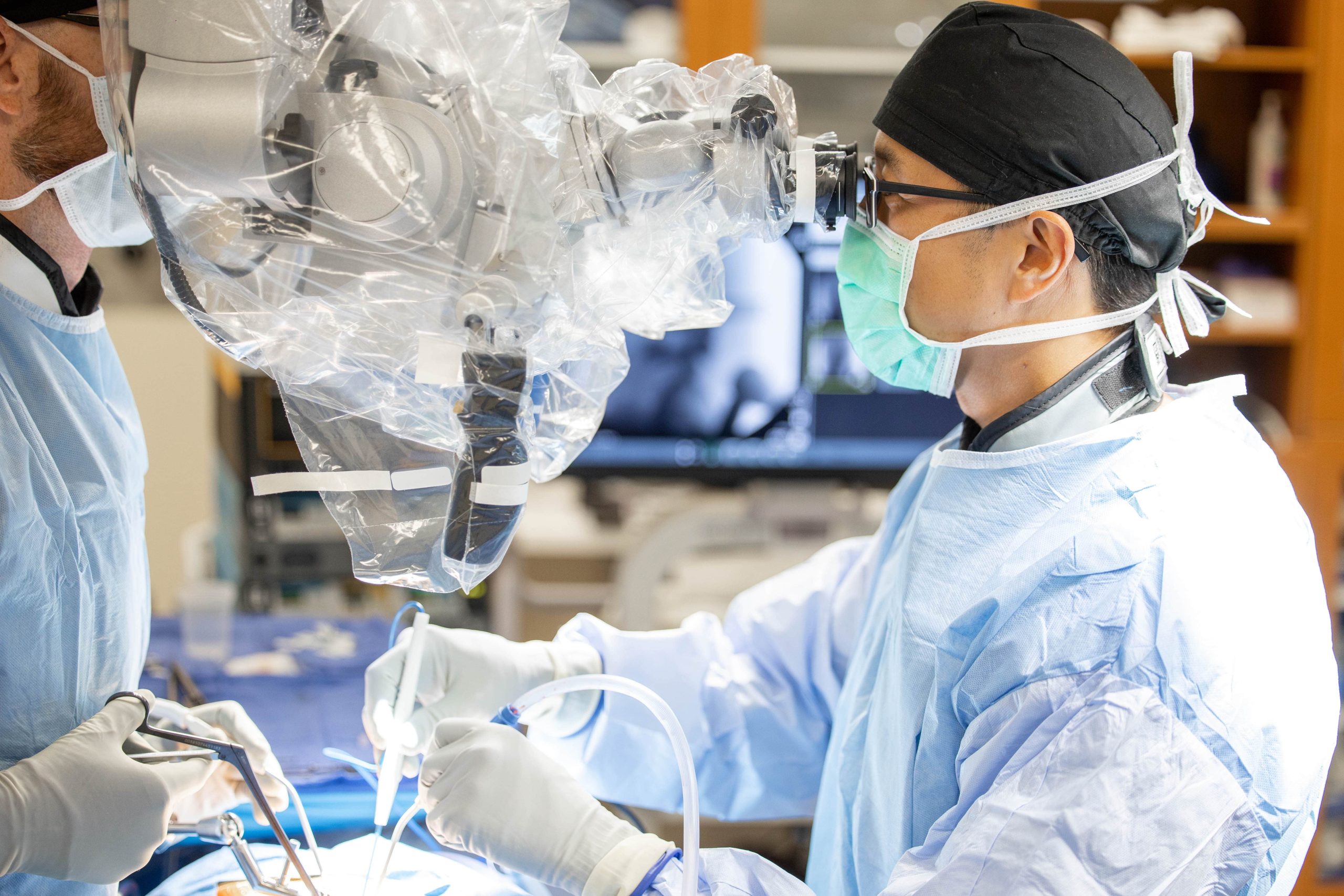
Our expert surgeons can perform MISS on the cervical and lumbar regions of the spine. Learn more about the procedures for these areas below.
The cervical region of the spine refers to the vertebrae in the neck. The MISS techniques available for this area include:
Surgery to remove a degenerated or herniated disc in the neck and fuse the two vertebral bodies together.
A procedure to completely remove and replace a diseased cervical disc with an artificial one.
Treatment for cervical stenosis of any cause, removing the lamina to relieve the upper spinal cord of its narrowed pressure.
Procedure to alleviate pain or weakness caused by a pinched spinal nerve root.
Commonly performed on patients with a fracture or instability by fusing the vertebrae to protect the spinal cord. Titanium screws and connecting rods are used to stabilize the vertebrae segment to allow a bone fusion to occur.
This surgery is similar to a laminectomy but without lamina removal. A laminoplasty creates a hinge on one side of the lamina, and a metallic plate is placed on the other side of the spine to make space.
The lumbar region is the lower back area of the spine. We can address lumbar conditions through the following procedures:
Surgery to relieve pressure and pain on spinal nerves in the spinal canal in your lower back.
Surgical procedure that addresses spinal stenosis by relieving pressure on spinal nerves.
A surgical procedure to remove a degenerative lumbar disc and implant an artificial replacement.
A surgery to permanently fuse two or more vertebrae in your spine, eliminating motion between them.
An advanced form of spinal fusion surgery with a shorter recovery time.
The candidacy for minimally invasive spine surgery depends on several factors, including the specific condition being treated, the patient’s overall health, and the surgeon’s expertise. Generally, the following individuals may be considered candidates for minimally invasive spine surgery:
It’s important to note that a qualified spine surgeon makes the decision to perform minimally invasive spine surgery on an individual basis after a thorough evaluation of the patient’s specific condition and medical history.
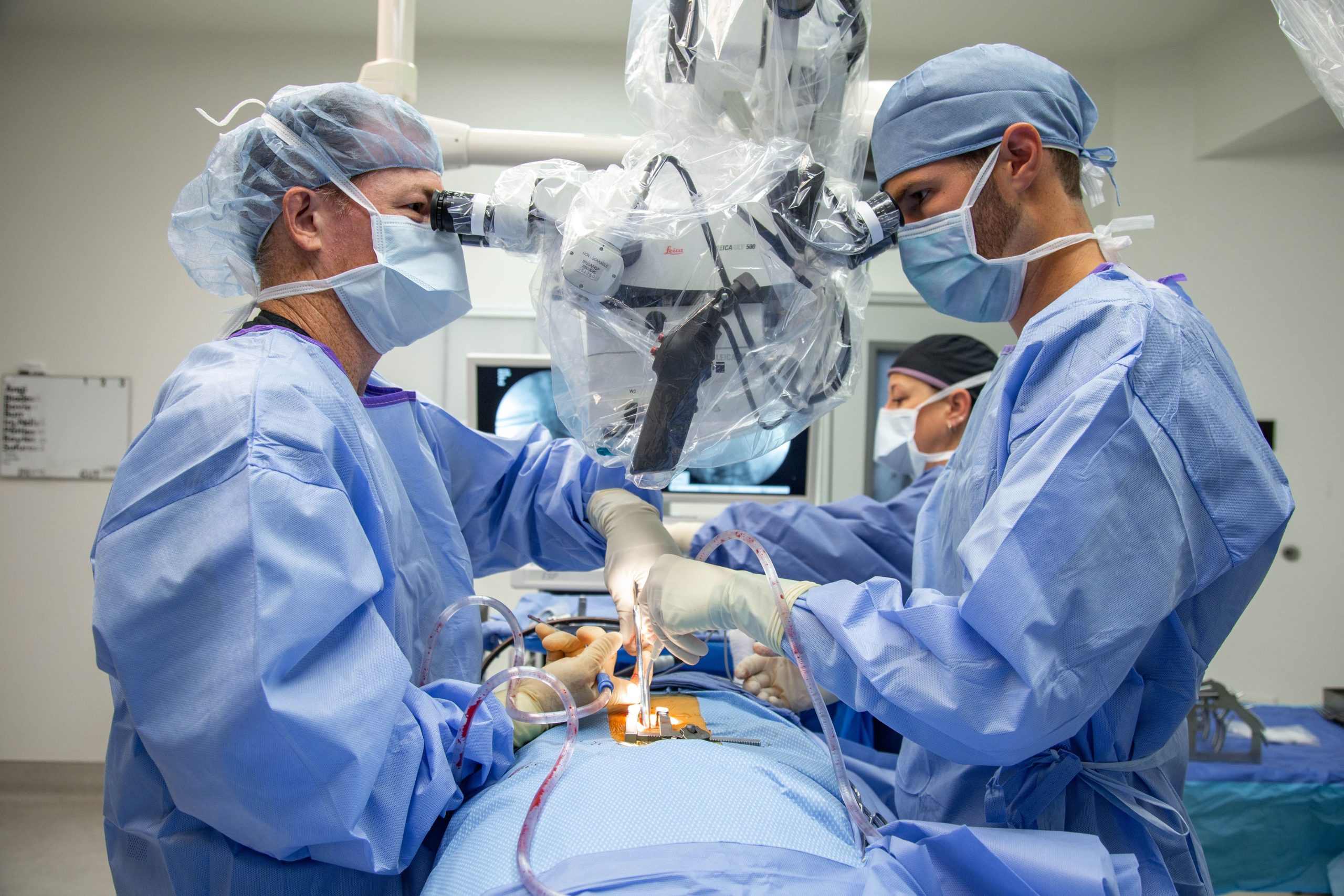
Spine surgery can far outweigh living with pain and the diminishing quality of daily life. For every possible risk of MISS, there are even more benefits compared to open surgery.
Minimally invasive spine surgery is effective at relieving pain for carefully selected patients. Some key benefits include MISS being less traumatic, having fewer complications than open surgery and causing considerably less pain.
Once you and your surgeon agree that minimally invasive spine surgery is the proper treatment, there are a few things that you can begin planning for a successful outcome. The following are some important things you can do to prepare:
Smoking affects your body’s ability to heal after surgery. Smoking can reduce your bone density or, in the case of a spinal fusion, your bones’ ability to fuse. Ask your doctor for help, as some medications can help you stop. Quitting smoking can reduce your risk of complications during the procedure. Having surgery may be the motivation to finally quit smoking.
Exercise can help your body and muscles stay in shape. A healthy body and strong core muscles can shorten your recovery time to return to an active lifestyle.
For those who are overweight, losing a few pounds before surgery can relieve pressure on the spine and ease recovery. Any weight loss plan should be discussed with your surgeon or a qualified dietician. Allow yourself ample time to plan weight loss before your scheduled surgery.
Your surgical team will review all the medicines you are taking and recommend which ones must be stopped before surgery. You may have to stop any nonessential medications and herbal therapies. These medications may interfere with anesthesia or other medications you may be given.
The more informed you are about your condition and your surgeon’s surgical plan, the better your expected outcomes will be.
Ask your surgeon when you can return to work (administrative vs. manual labor).
The recovery time with minimally invasive spine surgery is significantly shorter than traditional open surgery. Depending on your general physical health and MISS procedure, full recovery can be two to six months. Post-operative pain should be controlled with medication so that you can go home the same day or the next day.
Here is a general list of dos and don’ts after surgery to facilitate an optimal recovery:
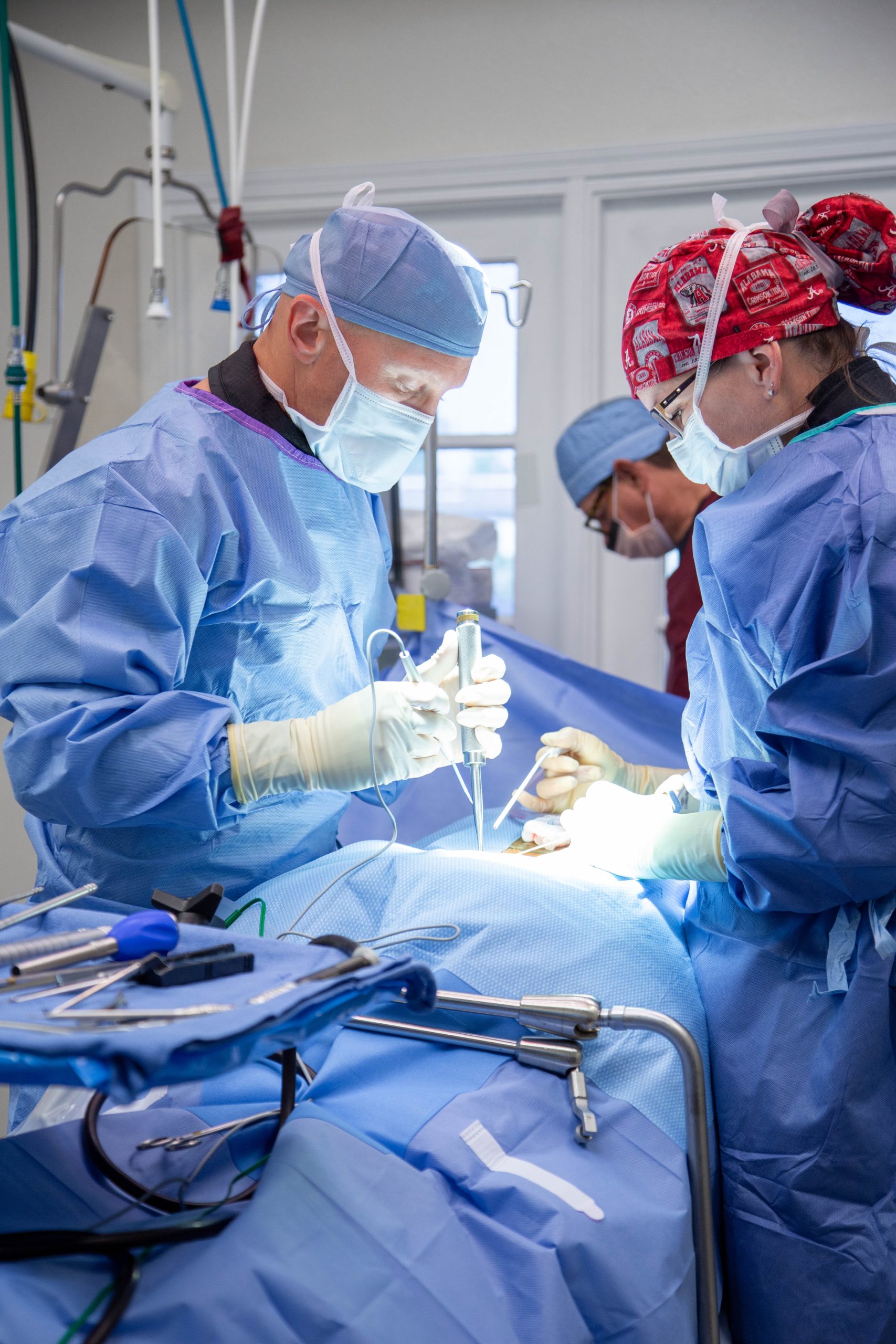
On average, someone who undergoes MISS can have a hospital stay of one to two days. However, there can be some exceptions to this rule. An individual can go home the same day for MISS decompressive surgery, whereas MISS fusion patients stay overnight or for two days. Most patients feel comfortable returning to administrative work after two to three weeks. After four weeks, a surgeon will generally clear decompressive surgery patients for physical activity. A MISS fusion usually has patients returning to their physical activities in around eight weeks.
Results can vary for every individual. Young, healthy and active individuals may have a shorter recovery time than elderly, overweight or inactive patients.

Recovering from back spine surgery is never an easy process. Patients should expect mild to moderate discomfort and physical limitations during recovery while their body heals.
One should be prepared to know the difference between normal discomfort after back surgery and when something is wrong.
The following signs might warrant a call to your spine surgeon’s office. Call your doctor immediately if you notice any of these signs or symptoms following surgery.
DISC exists to provide patients with long-term pain relief and improved physical function from their spinal conditions. You can trust us because:
For more information or questions about minimally invasive spine surgery, contact Desert Institute for Spine Care today.
Our spine health blog features up-to-date spine education and expert spine tips from our spine specialists here at DISC.
1635 East Myrtle Avenue Suite 100, Phoenix, AZ 85020, USA
18700 North 64th Drive Suite 105, Glendale, AZ 85308, USA
8630 East Vía de Ventura Suite 210, Scottsdale, AZ 85258, USA
3487 South Mercy Road, Gilbert, AZ 85297, USA
1635 East Myrtle Avenue Suite 400, Phoenix, AZ 85020, USA