April 28, 2026
Is Endoscopic Spine Surgery Safe?
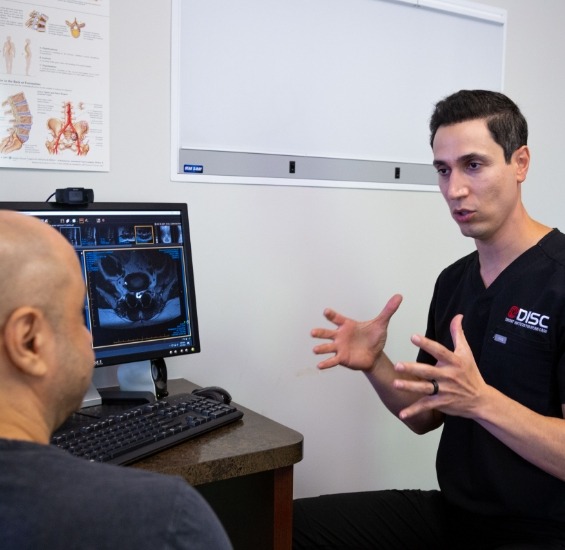
April 28, 2026
What to Look for in an ADR Surgeon

April 20, 2026
Why Some Surgeons Recommend ADR Over Fusion

April 16, 2026
Differences Between Laminectomy, Microdiscectomy and Laminotomy

April 15, 2026
Endoscopic Surgery vs. ADR

March 26, 2026
What Is Endoscopic Decompression?

March 26, 2026
Why Some Surgeons Don’t Offer Endoscopic Surgery
March 20, 2026
Endoscopic vs Minimally Invasive Spine Surgery

March 2, 2026
Desert Institute for Spine Care SurgeonsNamed Phoenix Magazine Top Doctors 2026
The Desert Institute for Spine Care (DISC) is proud to announce that Dr. Christopher Yeung,MD; Dr. Justin Field, MD; and Dr. Nima Salari, MD have been recognized as PhoenixMagazine Top Doctors 2026—a distinguished honor that reflects their continued leadership,innovation, and commitment to delivering exceptional spine patient care in Phoenix andthroughout Arizona. This year’s award is […]