
For many people, back pain feels like a normal part of life. It’s estimated that 75% to 85% of Americans experience back pain at some point. Back pain appears in different forms, ranging from a dull ache to shooting pain. Most back pain occurs in the lower back, known as the lumbar region. Half of patients with low back pain episodes will experience recurrent episodes in a year.
While most back pain resolves on its own and isn’t a sign of something serious, it should be looked at by a doctor in some cases. Your back consists of a spine, muscles, tendons and nerves, so it can be hard to figure what’s causing the pain on your own. If you don’t know what’s causing the pain, you won’t know how to treat it.
By going to a doctor for back pain, you can take steps toward feeling better again. A doctor who specializes in spinal conditions can determine the cause of your pain and initiate an effective treatment. They can also treat a condition that might otherwise get worse with time.
So, how do you know when you should see a doctor about lower back pain? Let’s look at common causes of back pain and symptoms that call for a professional examination.
Many different factors can cause or contribute to back pain, from injuries to various diseases. Patients might remember a specific incident that led to their back pain or have no idea what’s causing their discomfort. While there are dozens of conditions that can make someone’s back hurt, some are much more common than others.
Here are common causes of back pain:
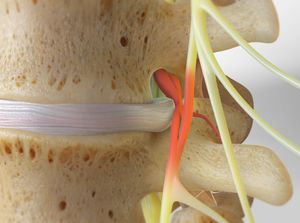
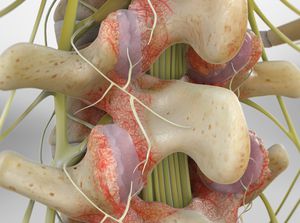
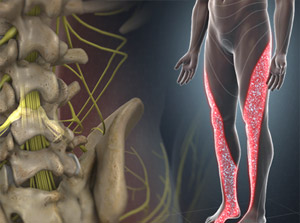
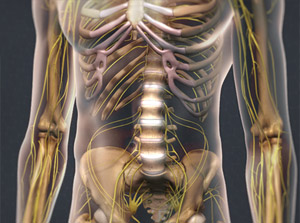
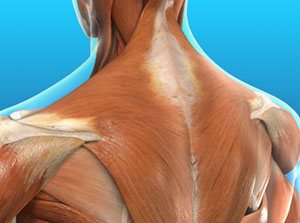
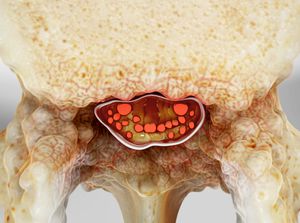
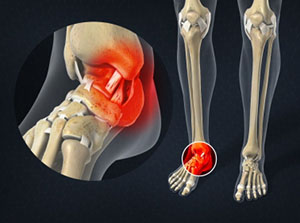
Some of the following are less common causes of back pain but worth considering if you’re concerned about your symptoms:

As mentioned earlier, most back pain improves in a few weeks with self-care and isn’t a cause for concern. Still, back pain can be debilitating, and some patients need a doctor’s help to cope with the pain or treat the problem with nonsurgical or surgical techniques. Back pain also can sometimes be a sign of a serious medical condition.
It’s a good idea to visit a doctor if you’re experiencing the following:
1. Nighttime Pain
For some people, lying down in bed makes their back pain worse, no matter what position they’re in. They might not have any back pain until they go to bed. Although nighttime back pain may be caused by common conditions like a sprain or scoliosis, it can be due to something serious, like an infection, fracture, nerve compression or spinal tumor. You should always get looked at by a doctor for any condition that disrupts your sleep.
2. Weakness, Numbness or Tingling
If you’re experiencing numbness, weakness or tingling with your back pain, you could have nerve damage or irritation. You should go to a doctor for nerve pain if it persists, especially if OTC pain relievers don’t help. If nerve pain does not get treated, it can lead to permanent damage.
3. Fever
A fever, along with back pain, can mean there’s an infection. Spinal infections include vertebral osteomyelitis, meningitis or a spinal epidural abscess. Spinal infections require immediate medical attention.
4. Unexplained Weight Loss
Unexplained weight loss along with back pain can be a sign of something serious. For example, weight loss and back pain are both symptoms of endocarditis. Endocarditis is inflammation of the heart’s inner lining and is a life-threatening condition. It’s rare in people with healthy hearts, but if it occurs, it requires emergency care.
Weight loss with back pain can also be a sign of cancer. Although spinal tumors are rare, you’ll still want to get checked by a doctor if you have unexplained weight loss with back pain.
5. Chronic Pain
If you’ve been experiencing back pain for more than a week, you should go to a doctor. A doctor can provide treatment to soothe symptoms and keep your back pain from becoming something serious.
6. Bowel or Bladder Control Problems
Severe low back pain with incontinence can be a sign of a rare but dangerous disorder called cauda equina syndrome. Cauda equina syndrome happens when nerve roots at the end of the spinal cord are compressed, affecting motor and sensory functioning. It may be caused by a large herniated disc in the lumbar region. Other possible causes include a spinal tumor or lesion, an infection or a violent injury.
Cauda equina syndrome is considered a medical emergency. If left untreated, it can lead to permanent paralysis.
7. Severe Pain
When should you go to a doctor for severe back pain? If your symptoms include severe back pain, you should visit a doctor, especially if the pain does not get better with rest or worsens over time. Likewise, if you experience back pain that shoots down your leg, you could have a damaged disc and should have a doctor evaluate you.
Even if you don’t have any of the above symptoms but experience back discomfort that disrupts your life, you should go to a doctor.
If back pain keeps you from doing the activities you enjoy or causes you significant discomfort, know that many different treatments are available to help you feel better. Back pain treatment falls under the following two categories:
Your doctor will likely recommend nonsurgical treatments for back pain before surgical options unless you have a serious condition. For example, they might suggest trying OTC pain relievers or topical creams first. They may prescribe a muscle relaxant if OTC medicines do not help.
If you continue to have pain after taking medicine, your doctor will recommend other nonsurgical treatments to relieve symptoms and restore functioning. For instance, they might administer a facet joint injection, which consists of local anesthesia and steroids and helps reduce inflammation and relieve pain. Facet joint injections produce results that can last for months.
Usually, back pain can be treated successfully with nonsurgical options, but sometimes an injury or spinal condition requires surgery. A doctor might recommend surgery if other treatments do not work first. A doctor might also suggest surgery to treat bone spurs, a spinal infection, a fracture, a tumor or a degenerative spinal condition that’s causing problematic symptoms.
Learn More About At Home Remedies for Back Pain
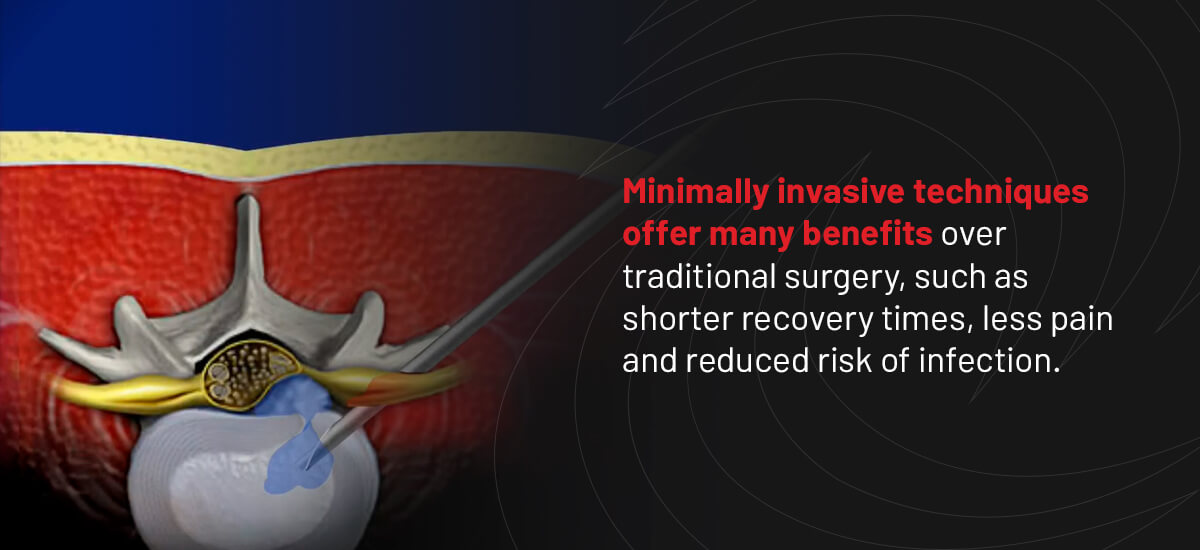
If the idea of back surgery makes you feel nervous, know that there are a range of innovative, minimally invasive procedures available. Minimally invasive techniques offer many benefits over traditional surgery, such as shorter recovery times, less pain and reduced risk of infection.
One example of a least invasive surgical treatment is a Selective Endoscopic Discectomy™. This procedure involves a small incision and a thin endoscope to treat a herniated disc.
If you’re still wondering if you should see a doctor for back pain, the short answer is yes. Going to the doctor for your back pain can help you find relief so you can enjoy life once again. At the Desert Institute for Spine Care (DISC), you can rest assured our doctors and staff will take good care of you.
At DISC, we believe every patient deserves compassionate, personalized care. We developed Personalized Pain Diagnostics (PPD) to identify the pain generator and most accurate diagnosis. With PPM we can personalize and tailor the right treatment or surgical option for our patients. We begin by asking questions and listening carefully to your experience. We then investigate your symptoms further through an examination and imaging tests.
Once we develop ideas about your pain, we will discuss them honestly and clearly with you and invite you to ask questions. We want to ensure you feel comfortable and can make an informed decision about your treatment.
When you’re ready, we’ll apply the latest technology to treat your pain and help you restore your lifestyle.
To learn more about our innovative treatments for back pain or schedule an appointment, please fill out our contact form or call one of our Phoenix-area locations today.
